The year 2025 wasn’t easy for most ACOs struggling with the sudden transition to data aggregation. In fact, it was a trial by fire. ACOs joined the modern era of quality reporting in 2025 with APP (APM Performance Pathway) Reporting, which spurred aggregation from multiple practice systems and patient matching across the ACO. This required […]
How ACOs Can Manage Both Total Cost of Care and Episodic Payment Models
It’s a new world for ACOs, especially those just immersing in aggregated patient data. Once a rarity for ACOs to look beyond claims data for population health and analytics, ACOs are now finding themselves at the center of a data need surge. The transition from easy, manual quality reporting for a sample of ACO patients […]
What TEAM and ASM Tell Us About the Future of Value-Based Care
In the last year, CMS has made strides to revamp health care through Medicare and Medicaid, taking some controversial steps. But one of their more positive moves involves changes to their Value-Based Care strategy. So, what does that strategy—through new or restructured payment models—tell us about where the system is headed? TEAM, ASM, ACCESS and […]
Why ACOs Should Create High-Performance Specialty Networks
Specialty costs have been a difficult problem for ACOs, driving a huge portion of total costs in specialty-driven services of all kinds: physician visits, hospital admissions, procedures, and treatments. ACOs have argued they don’t have the tools needed to combat costs. But that is not quite true. We argued in a recent webinar that ACOs […]
Discover Cost Drivers in TEAM Surgeries
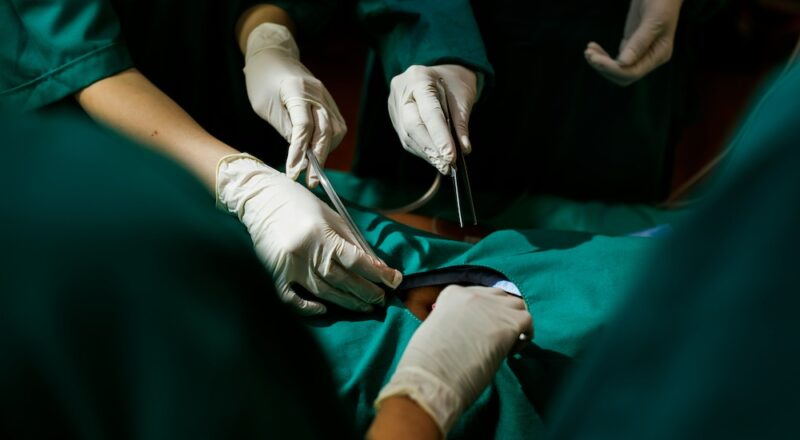
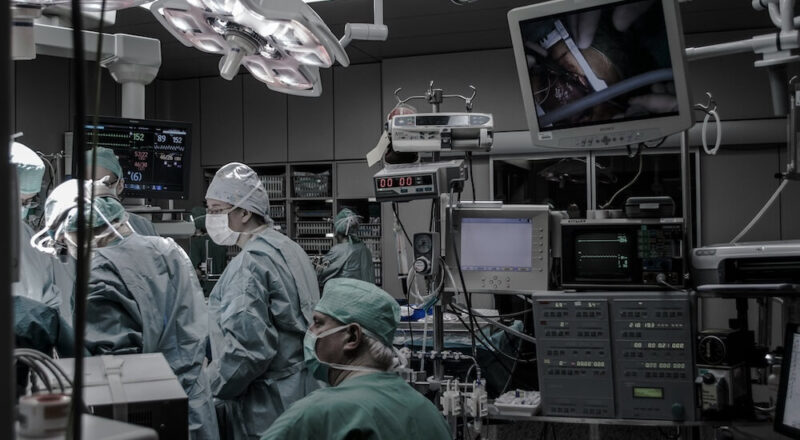
The CMS TEAM payment model focuses on the patient surgery and recovery process, which puts hospitals at risk for both cost and quality of surgeries. The end result of TEAM, if implemented well by hospitals and clinicians, is benefits for patients, with more coordination of services and fewer complications. The American College of Surgeons supports […]
Rethink the Essential Role of Primary Care Physicians in TEAM
With TEAM’s focus on improving surgical recoveries and costs in major hospital-based surgeries, it’s easy to miss the importance of primary care physicians. But their role is essential for meeting TEAM’s objective to improve patient recovery and lower costs in the five major types of surgery covered by TEAM. And perhaps not in the way […]
For TEAM Success, Collaboration Agreements Must Be a Win-Win for Specialists and Hospitals
The new Transforming Episode Accountability Model (TEAM) targets the highest cost or volume surgeries in the Medicare program. While hospitals bear the financial risk, CMS has created a vehicle to align interests with other providers through Collaboration Agreements that can include financial incentives. How those are structured will be key to the successful alignment—or fracture—of […]
New TIPS for TEAM: Adopt ERAS Guidelines for Prevention of Complications and Faster Recovery
If TEAM has your hospital searching for an evidence-based toolkit to improve surgical outcomes and reduce recovery time, participating hospitals and their surgical teams should pay heed to ERAS (Enhanced Recovery After Surgery) protocols. The guidelines are tailored to more than twenty types of surgery as well as anesthesia and intensive care. They have been […]
TIPS for TEAM: How to Reduce the Top Driver of Higher Variable Costs in Surgery Episodes
One of the largest and most significant changes to specialty care payments in Medicare commences in January. TEAM (Transforming Episode Accountability Model) is poised to put hospitals at risk for total costs of care for the highest cost Medicare surgical episodes, including Coronary Artery Bypass Graft (CABG), Lower Extremity Joint Replacements (LEJR), major bowel procedures, […]
Three Strategies for ACOs to Optimize Specialty Care through TEAM
Both the greatest strength and weakness of the ACO shared savings (MSSP) model is its focus on primary care, particularly chronic disease. ACOs have put patients with diabetes, hypertension, and other conditions usually handled through primary care physicians at the center of care coordination, population health, and care management. But as CMS Value-Based Care’s central […]